 |
| National Botanic Garden of Wales, May 2013 |
There are a very few centres in the country where this type of work is done. The islets in question are the Islets of Langerhans, which are the structures within the pancreas that contain insulin-secreting beta cells. The research team extract clumps of islet cells from cadaveric donor pancreata* by dissolving away the tissue around the islets, and then infuse them (sometimes on several occasions) into the hepatic portal vein of the recipient. The islets are transported to the liver and lodge in the tissue there, and somehow a blood supply is created from nowhere (vascularisation) to nourish them and to transport away the insulin that they manage to secrete. The fact that any of this works seems to me to be a miracle, much like throwing mortar and bricks randomly into house foundations might cause a habitable bungalow to emerge.
Although the techniques are still experimental, islet transplantation is approved for patients within the NHS. Recipients are very few (208 worldwide, 34 in the UK), partly because donors are very few, and partly because the selection criteria are so stringent. Most qualify due to severe hypoglycaemia unawareness, which can be utterly debilitating, leading to incapacitating hypoglycaemia with no warning. Others might be suitable recipients because they are already taking lifelong immunosuppressant medication following a kidney transplant.
The success rate of islet transplants is improving, measured by independence from insulin injections, but only 10% of transplant recipients are still insulin-independent after 5 years. It seems, however, that even though they have to return to insulin injections, some recipients recover their awareness of hypoglycaemia, which is a huge bonus. The researchers at IRL are following a number of strands of research: improving the yield of islets from donated pancreata (they only get about 50% yield at the moment), improving the vascular development and survival of implanted islets, and enhancing the immune protection of islets. They are also thinking about different sites for implantation - the pancreas is deemed too 'brittle' for implantation, which is why the liver is used, but there are other options that may be more successful, such as the intestinal submucosa.
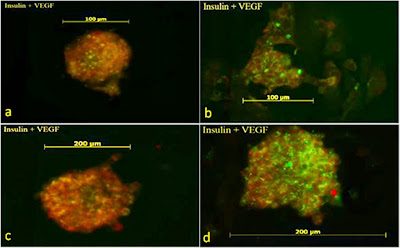
Extraction of islets is quite brutal, so it makes sense to try to improve their 'health' before transplantation. It has been found that they survive better if held in a rotational suspension rather than allowing them to settle in culture. Next, ways to enhance vascularisation include stimulating secretion of vascular endothelial growth factor (VEGF) through incubation of islet cells with various drugs that not only increase VEGF expression but have also been shown to up-regulate beta-cell insulin secretion (the 'glitazones' or thiozolidinedione family).
Progress is slow in research, and while I thoroughly approve of what they do, I can't imagine doing it myself - hardly any human contact, tens of years before results of experiments are any practical use. They also struggle for funding, ethical approval of research, and lack of donor material. Research labs are only third in line for any pancreas donation - first are medical centres that do whole pancreas transplants, and second are those that perform islet transplantations on people rather than just doing research. So IRL ends up with the pancreases that nobody else wants.
We all sang rousing songs in the minibus on the way back (no, of course we didn't) but I was mystified by those of the party, and there were several, who had been on this trip more than once. The rate of progress meant that aside from the benefit of tea and biscuits and sitting down for an hour or so, there would have been little change since the last time they were there. But then, this group contains individuals that are like none I have ever met before.
* by far my best moment of the evening came when the lead researcher first used 'pancreata' as the plural of pancreas.
Here's a song you might have sung on the bus:
ReplyDeletehttp://www.com-www.com/weirdal/pancreas.html
It is really excellent apart from the bit where he says the force between his pancreas and any other pancreas is inversely proportional to the distance between them. I think it should be the distance squared. This spoils an otherwise perfectly good song about a pancreas.
p.s. sorry to be commenting on the one before the one you said you wanted comments on.
And here's a link to the song being performed: http://youtu.be/tqDBB0no6dQ.
DeleteVery exciting. I won't point out the other physiological inaccuracies in the song, in case it spoils it further.